On December 1st each year the world unites to commemorate World AIDS Day to support those living with HIV and honor the memory of those who died from AIDS-related illnesses. This year’s theme is “Equalize” to inform people globally of inequalities as one of the growing challenges. Enormous progress has been made in the treatment, care, and prevention of HIV/AIDS in the past 40 years with fewer people becoming infected. Those who do are healthier and now living longer. In the US, HIV incidence decreased from the highest number of infections, 130,400 in 1984 to an estimated 35,000 in 2019, with a gender distribution of 81% male and 19% female.
CDC estimates an 8% decrease in the overall number of new HIV infections since 2015 and is suggestive of two key factors: The first is the development of new therapies that can suppress HIV more effectively. The second is the introduction of pre-exposure prophylaxis (PrEP) therapy. In 2012, the FDA approved the use of antiretroviral medications used in the treatment of HIV infection, to additionally prevent infection in men and women who were not yet diagnosed with HIV. Pre-exposure prophylaxis treatment or PrEP is a protocol that uses certain HIV medications* prescribed specifically to prevent infection and is continued throughout periods of potential exposure in persons at risk. In HIV-uninfected patients, PrEP therapy is an evidence-based approach to prevent new infections among those at greatest risk. This approach can reduce the risk of HIV transmission by greater than 90 percent when patients are adherent with consistent use.
Recently, about one-quarter of people who are eligible for PrEP are now prescribed this treatment, a substantial improvement from only 3% five years ago, however, for women specifically, based on 2019 CDC statistics, only 10% who were eligible were prescribed PrEP. At PurpleLab, we looked at this further using our HealthNexus platform and recent 5 years of commercial data to understand potential variation in gender distribution among patients taking PrEP therapy.
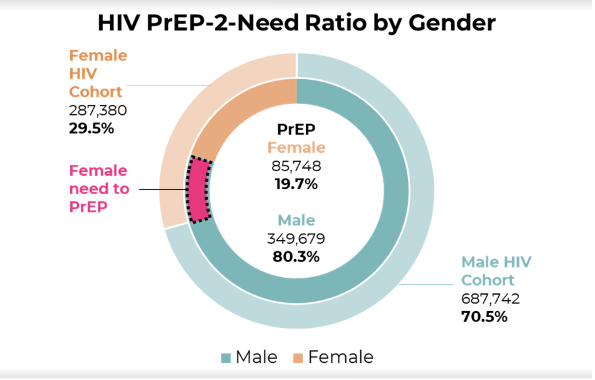
Our data shows an increase in awareness and use of PrEP related to the need for treatment, however, we found there are gaps between men and women. In this data analysis, distributions for people with an HIV diagnosis is 70.5% for men and 29.5% for women, yet men have a higher rate of PrEP, 80.3% compared to 19.7% for women. This data reinforces the need for:
- Programs, public health agencies and provider groups who can effectively promote awareness and reach those in need of PrEP.
- Improved PrEP medication adherence in eligible patients
- Better understanding of those at risk for new HIV infection and transmission
- Better patient education about benefits of PrEP treatment and management of possible adverse effects
- Providers who have a wider range of practice settings that can reach high risk patients for PrEP
- Improved patient access to resources for assistance navigating treatment options and financial assistance.
Additional patient, provider information and resources are available:
- The World Health Organization: https://www.who.int/health-topics/hiv-aids#tab=tab_1,
- Centers for Disease Control and Prevention cdc.gov/hiv/risk/prep/
- The CDC’s “Let’s Stop HIV Together” campaign, https://www.cdc.gov/stophivtogether/index.html to end the HIV epidemic through “Ending the HIV Epidemic in the U.S. (EHE) initiative and the National HIV/AIDS Strategy”: https://www.cdc.gov/hiv/group/gender/women/prep-coverage.html, an evidence-based campaign aimed at empowering communities, partners, and health care providers to reduce stigma, promote testing, prevention, and treatment of HIV.
- Patient therapy and support programs sponsored that help with access to HIV treatment and HIV prevention medication: https://www.gilead.com/purpose/medication-access/us-patient-access
*(PrEP) includes tenofovir disoproxil fumarate-emtricitabine, tenofovir alafenamide-emtricitabine, and oral and injectable cabotegravir.
References in order of use:
https://www.hiv.gov/events/awareness-days/world-aids-day
https://www.unaids.org/en/World_AIDS_Day
https://www.cdc.gov/hiv/statistics/overview/index.html
https://www.cdc.gov/nchhstp/newsroom/2021/2019-national-hiv-surveillance-system-reports.html
https://www.cdc.gov/hiv/statistics/overview/diagnoses.html
https://www.cdc.gov/hiv/risk/index.html
https://www.cdc.gov/hiv/clinicians/prevention/prep.html
Mayer, KH., et al. Administration of pre-exposure prophylaxis against HIV infection. In: UpToDate, Sax, PE. (Ed), UpToDate, Waltham, MA. (Accessed on November 3, 2022)